|
9/13/2023 0 Comments Transmission of hepatitis aMelissa Jenkins, chief of the division of infectious diseases at MetroHealth, in Cleveland, Ohio.Ī research article published recently in the journal Pathogens noted that the opioid epidemic and less access to health care have also fueled new hepatitis C cases. "Before 1993, a blood transfusion was a common way to get hepatitis C, but now blood transfusion is safe because we check the blood," explained Dr. Organ transplants and blood transfusions.Health care worker exposure to blood-borne infections.Sharing medical and other items, such as glucose monitors and razors that have infected blood on them.Sex with someone infected with the virus, which is reported more among men who have sex with other men.Tattoos and piercings, especially from unlicensed and unregulated establishments.Birth: approximately 6% of children born to infected mothers are also infected.Sharing of drug needles or other injection materials.Centers for Disease Control and Prevention, hepatitis C transmission occurs when you come into contact with the blood of someone who is infected. They will also explain if there's a hepatitis C vaccine, and what medications are used to treat this viral infection.Īccording to the U.S. To help you protect yourself against this virus, liver experts describe how you get hepatitis C, if it's curable and how contagious it is. Local health jurisdictions: notifiable to the Washington State Department of Health (DOH) Communicable Disease Epidemiology (CDE) within 7 days of case investigation completion or summary information required within 21 days.The American Liver Foundation estimates that it affects about 2.7 million people in the United States today.Laboratories: notifiable to local health jurisdiction within 24 hours submission on request – specimen associated with positive result, within 2 business day.Health care providers and Health care facilities: notifiable to local health jurisdiction within 24 hours.To educate cases and contacts about transmission of hepatitis A and how to reduce their risk of infection.To educate contacts about signs and symptoms of disease, to facilitate early diagnosis. 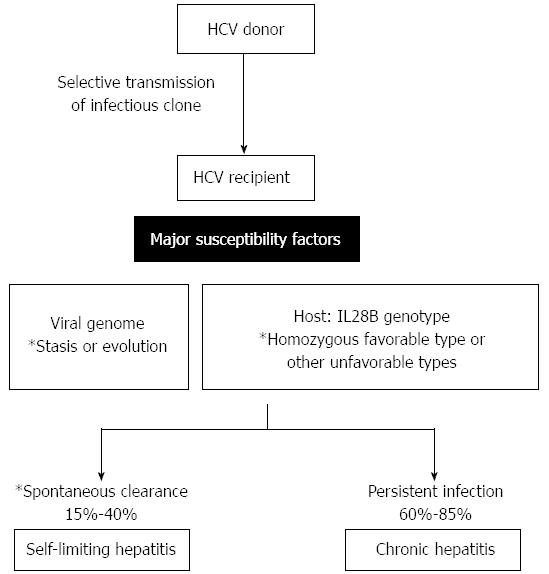
To identify contacts and assure timely prevention measures.To identify individual cases, disease outbreaks and potential sources of ongoing transmission to prevent further spread of hepatitis A.Recent Washington trends: Since 1989 when there were 3,273 cases, hepatitis A incidence decreased to fewer than 100 cases a year with increased vaccination. Prevention: To prevent infection, immunize all children and any adults with risks for exposure including travel to endemic areas. Transmission can occur with groups having poor hygiene or fecal-oral sexual practices. Bloodborne transmission is very rare.Īdditional risks: Infected young children may have no symptoms but can be communicable. Recent outbreaks in this country have been associated with imported produce. 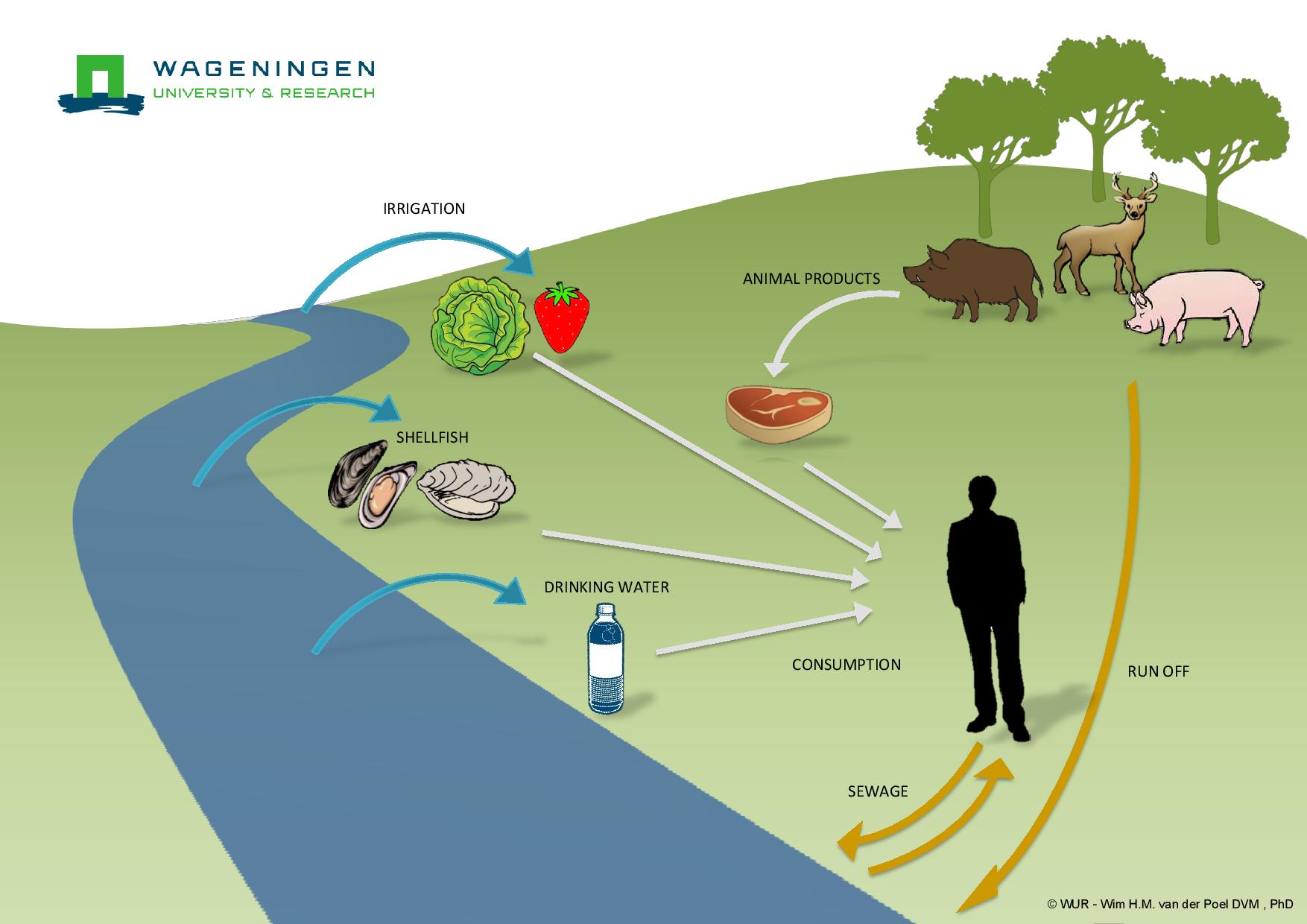
Sources: Acutely infected humans shed virus in the feces and transmit directly or through fecally contaminated food (produce, shellfish, uncooked items), water, and environment, often encountered during international travel. Almost all cases recover but rare infections are fatal or require liver transplantation. 
Cases may be asymptomatic, particularly in children. Illness and treatment: Onset is usually abrupt with fever, nausea, and abdominal pain followed by jaundice.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
